Picture this: you live 90 minutes from the nearest hospital, your family doctor retired last year, and there’s still no replacement when your elderly parent needs emergency care at 2 AM, every minute counts.
However, nearly 200 rural hospitals in the U.S. have closed over the past two decades, resulting in millions of Americans lacking access to emergency rooms, inpatient care, and other critical services. This scenario plays out thousands of times daily across rural America and communities worldwide.
The Reality Behind Rural Healthcare Challenges
Rural healthcare systems face a perfect storm of challenges that go far beyond simple distance barriers. While most discussions focus on obvious issues like provider shortages and hospital closures, the real crisis lies in how these factors create cascading system failures.
Geographic and Infrastructure Barriers Create Care Deserts
Rural geography creates natural barriers that urban healthcare systems never face. The distance to the nearest hospital varies significantly, ranging from 3.4 to 23.9 miles for average rural Americans. But distance is only part of the equation – poor road conditions, unreliable vehicles, and weather restrictions can make even nearby facilities unreachable during critical moments.
Infrastructure challenges extend beyond transportation. Approximately 14.5 to 21 million rural Americans can’t access broadband internet capable of supporting telehealth services. This digital divide particularly impacts elderly populations who could benefit most from remote monitoring and virtual consultations, creating a cycle where those who need care most can’t access modern delivery methods.
Economic Pressures Force Difficult Healthcare Choices
Rural health care economics operate on razor-thin margins that make sustainability nearly impossible under current models. Rural hospitals serve populations with higher uninsured rates and greater reliance on Medicaid, which typically reimburses at lower rates than private insurance. This creates a vicious cycle where reduced revenue leads to service cuts, driving patients elsewhere and further reducing financial viability.
The ripple effects extend beyond hospitals themselves. When rural healthcare facilities struggle financially, they often reduce services, cut staff, or delay equipment upgrades. All of these decisions drive qualified healthcare professionals to seek opportunities in better-resourced urban settings, creating a brain drain that leaves communities with aging provider workforces.
Provider Shortage Crisis Threatens Long-term Viability
The rural provider shortage represents more than inconvenience – it’s an existential threat to community sustainability. Rural areas have 39.8 physicians per 100,000 residents compared to 53.3 in urban areas. However, raw numbers don’t capture the full picture of overworked rural providers who typically work longer hours and cover broader scopes of practice.
Medical school graduates face significant financial pressure to choose high-paying urban specialties over lower-compensated rural practice. The average medical school debt exceeds $200,000, making rural family medicine positions financially unattractive compared to urban specialty roles that can pay two to three times more. Without systematic interventions, this trend will worsen as healthcare costs continue rising faster than rural community incomes.
Beyond economic factors, rural healthcare access suffers from professional isolation that urban providers rarely experience. Rural practitioners often work without immediate specialist backup, handle diverse cases outside their primary training, and face community pressure to be available around the clock.
Technology Solutions That Actually Work in Rural Settings
Technology has evolved from a nice-to-have convenience to an essential rural healthcare lifeline, but success requires more than just video calling software. The most effective solutions integrate multiple technologies to create comprehensive virtual care ecosystems.
Telemedicine Becomes the Great Equalizer
Store-and-forward telemedicine, where healthcare data is collected and transmitted for later review, often works better in rural areas than real-time video consultations. This approach accommodates limited bandwidth, allows providers to review cases during optimal hours, and enables specialists to serve larger rural populations efficiently. Telehealth visits can help reduce avoidable emergency room visits and hospital readmissions, which is particularly valuable for rural residents who face long travel distances.
Through the Ontario Telemedicine Network, most First Nations communities across the province have virtual access to care. This success demonstrates that improving access to healthcare in rural areas is achievable when technology programs prioritize community engagement and cultural competency.
Successful rural telehealth programs also prioritize digital literacy training for both patients and providers. Communities that invest in technology training for elderly residents see 60% higher telehealth adoption rates, while providers trained in remote care delivery report greater job satisfaction and expanded practice capabilities.
Mobile Health Units Bridge Critical Care Gaps
Modern mobile health units go far beyond basic screenings – they’re essentially hospitals on wheels equipped with advanced diagnostic equipment, laboratory capabilities, and direct connections to urban medical centers. These units can perform everything from mammograms and cardiac stress tests to minor surgical procedures.
The key to mobile unit success lies in strategic scheduling and community partnerships. The most effective programs coordinate with local employers, schools, and community centers to maximize accessibility and reduce stigma. Mobile units that partner with local health departments and existing clinics report higher patient retention rates and better health outcomes.
Data connectivity enables mobile units to function as extensions of larger healthcare networks rather than isolated services. When mobile providers can access patient records, consult with specialists in real-time, and coordinate follow-up care, they become integral parts of comprehensive healthcare delivery.
AI and Remote Monitoring Transform Chronic Care Management
Artificial intelligence applications designed for rural healthcare focus on predictive analytics that identify health risks before they become emergencies. AI-powered systems analyze patient data from wearable devices, home monitoring equipment, and electronic health records to flag concerning trends that might escape notice during infrequent office visits.
Remote patient monitoring technology proves particularly effective for managing diabetes, heart disease, and hypertension – conditions that disproportionately affect rural populations. Patients using connected devices show 30% better medication adherence and 25% fewer emergency room visits compared to those receiving traditional care alone.
The most successful rural AI implementations focus on supporting rather than replacing human providers. AI tools that help rural practitioners make faster, more accurate diagnoses or identify patients needing urgent attention work best when they strengthen existing relationships between providers and communities.
Community-Based Healthcare Models That Scale
Community-driven approaches offer sustainable solutions that work within existing rural resources while building long-term capacity. These models recognize that effective healthcare access in rural communities requires more than just clinical services.
Community Health Workers Become Healthcare System Connectors
Community health workers represent one of the most cost-effective strategies for improving rural healthcare access, but their success depends on proper training, support, and integration with formal healthcare systems. Effective programs go beyond basic health education to include care coordination, chronic disease management, and navigation assistance.
The most successful rural programs recruit from within local communities, ensuring cultural competency and established trust relationships. Workers who share language, cultural background, and life experiences with their clients achieve significantly better health outcomes than external providers. Training programs that combine formal health education with community-specific knowledge create workers who effectively bridge medical and social service systems.
Technology amplifies worker effectiveness when properly implemented. Workers equipped with tablets or smartphones can access patient records, coordinate care with providers, and document interactions in real-time, transforming them from isolated volunteers into integral healthcare team members.
Public-Private Partnerships Create Sustainable Funding Models
Successful rural healthcare systems increasingly rely on innovative public-private partnerships that leverage diverse funding sources and expertise. These partnerships combine government resources, private sector efficiency, and community engagement to create financially sustainable healthcare delivery models.
Effective partnerships align incentives among all stakeholders rather than creating zero-sum competition for limited resources. When private companies, government agencies, and community organizations share both risks and rewards, they develop long-term solutions rather than short-term fixes that don’t address underlying problems.
The most innovative partnership models incorporate value-based payment systems that reward improved health outcomes rather than simply paying for services rendered. These arrangements encourage prevention-focused care that reduces long-term costs while improving community health.
Regional Healthcare Networks Maximize Resource Efficiency
Regional healthcare networks allow small rural facilities to share resources, expertise, and costs while maintaining local presence and community connections. These networks coordinate everything from specialist rotations and equipment sharing to joint purchasing agreements that reduce costs for all participants.
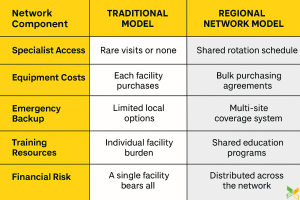
Successful networks balance centralization with local autonomy, ensuring that shared resources support rather than replace community-based care. Networks that maintain strong local identities while providing system-wide support achieve better patient satisfaction and provider retention than those emphasizing centralized control.
Technology enables network coordination that was impossible in previous generations. Shared electronic health records, centralized scheduling systems, and coordinated care protocols allow network members to function as integrated healthcare systems while preserving community connections that make rural healthcare unique.
Policy and Funding Strategies That Create Change
Effective rural healthcare policy goes beyond emergency funding to address structural inequities that create ongoing challenges. The most impactful legislation combines immediate relief with long-term system reforms that make rural healthcare financially sustainable and professionally attractive to providers.
Rural communities have proportionately fewer nurses than urban communities. For example, for every 10,000 rural residents, there are sixty-five registered nurses (compared to 94 registered nurses in urban areas) (https://online.regiscollege.edu/blog/rural-health-care). This disparity highlights the urgent need for targeted workforce development programs that address both recruitment and retention challenges.
Loan forgiveness programs for healthcare professionals serving rural communities prove effective when properly designed and funded. The most successful programs combine financial incentives with professional development opportunities, mentoring support, and pathways to permanent residency that address non-financial factors influencing provider retention.
With $50 billion allocated between fiscal years 2026 and 2030, the program is designed to stabilize and transform rural health systems nationwide by supporting infrastructure, workforce development, and innovative care delivery models. This substantial investment represents a significant shift toward prioritizing rural healthcare as a national concern.
Creative funding mechanisms like healthcare facility bonds, community ownership models, and cooperative purchasing agreements help rural communities maintain healthcare access even when traditional business models fail. Communities that successfully maintain healthcare facilities often combine multiple funding sources and governance structures to create resilient systems.
Emergency Preparedness and Crisis Response
Rural healthcare systems face unique vulnerabilities during emergencies – they often lack backup resources, have limited surge capacity, and may become completely isolated when transportation networks fail. However, rural communities that invest in emergency preparedness often develop remarkable resilience and mutual aid networks.
Effective rural emergency preparedness combines formal medical response capabilities with community-based support systems that can function independently when external help isn’t available. This includes training community members in basic medical skills, maintaining emergency supply caches in multiple locations, and developing communication systems that work when primary networks fail.
The COVID-19 pandemic highlighted both vulnerabilities and strengths in rural healthcare systems. Rural facilities that successfully managed pandemic challenges often had pre-existing relationships with regional partners, flexible staffing models, and strong community trust that enabled rapid adaptation to changing conditions. These lessons provide blueprints for preparing for future health emergencies.
Measuring Success and Continuous Improvement
Measuring rural healthcare success requires metrics that account for unique rural circumstances rather than simply applying urban healthcare benchmarks. Traditional metrics like patient volume or revenue per bed may not accurately reflect rural healthcare value.
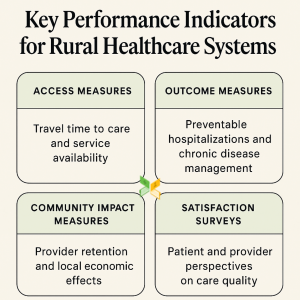
Continuous Quality Improvement in Resource-Limited Settings
Quality improvement in rural healthcare requires adaptable approaches that work within resource constraints while still achieving meaningful outcomes. The most effective rural quality improvement initiatives focus on high-impact, low-cost interventions that can be implemented and sustained with existing staff and resources.
Peer learning networks allow rural healthcare providers to share successful practices and learn from each other’s experiences without requiring expensive external consultants or formal research infrastructure. These networks often produce innovations that are immediately applicable to similar rural settings because they’re developed by providers facing similar challenges.
Regular community feedback mechanisms help rural healthcare systems stay aligned with local needs and priorities while identifying problems before they become crises. Communities with strong feedback systems report higher satisfaction with healthcare services and greater willingness to support local healthcare facilities.
Building Healthier Rural Communities Together
Building stronger rural healthcare systems isn’t just about fixing a broken system – it’s about creating innovative models that can serve as blueprints for healthcare delivery in challenging environments worldwide. The strategies outlined here represent tested approaches that real communities have used to overcome seemingly impossible odds.
Access to healthcare in rural areas improves when communities address root causes rather than just treating symptoms. Whether you’re supporting telemedicine expansion, volunteering with local health initiatives, or advocating for systemic change, every action contributes to building the stronger, more equitable healthcare systems our rural communities deserve. The technology exists, the funding is flowing, and the path forward is clear – now it’s time to act.
FAQs on Rural Healthcare Solutions
1. What funding sources are available specifically for rural healthcare improvement projects?
Rural healthcare projects can access USDA Rural Development grants, HRSA rural health programs, CDC rural health initiatives, and private foundation grants. The key is matching project goals with funder priorities and combining multiple funding sources.
2. What role do faith-based organizations play in rural healthcare delivery?
Faith-based organizations often serve as crucial healthcare access points, particularly for mental health services, health education, and care coordination. They frequently host health fairs, vaccination clinics, and support groups in rural communities.
3. What are the most common mistakes communities make when trying to improve rural healthcare?
The biggest mistake is pursuing quick fixes rather than sustainable system changes. Many communities focus on recruiting individual providers without addressing underlying factors that make rural practice challenging, such as inadequate infrastructure or unsustainable financing models.
